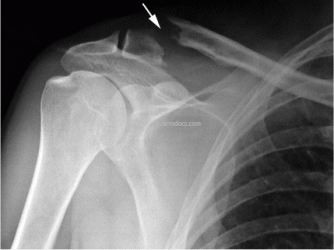
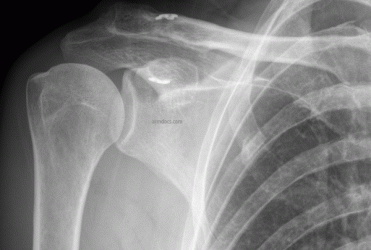
How is the procedure performed?
The procedure is performed under a combination of general and regional anaesthesia. The procedure may be performed with arthroscopic assistance or open. An incision is made over the outer end of the collar bone and the bone is exposed. A guide wire is drilled through the clavicle and in the coracoid process using a dedicated jig and its position confirmed with an x-ray machine. A tunnel is drilled over the guide wire. A suspensory device is placed between the clavicle and the coracoid and tightened to stabilise the coracoclavicular interval. In some instances it may be necessary to use a plate and screws to reinforce the fixation. At the end of the procedure the overlying muscles are repaired and the skin is closed with sutures placed deep to the skin.
Benefits
The main benefit of the procedure is to reduce the fracture, restore stability and improve the function of the joint.
Risks
Pain - The shoulder may be painful for some weeks after surgery. This is usually managed by taking appropriate pain relieving medication and activity modification.
Bruising – Bruising may occur around the joint and the scar and usually resolves 2-3 weeks after surgery.
Bleeding – A small amount of bleeding from the surgical wound is not unusual and will usually settle after a day or two.
Numbness around the scar: A small patch of numbness adjacent to the scar is not uncommon but does not cause any functional problems.
Hardware failure – Occasionally the sutures used in the tight-rope device may work loose or fail. This may result in further surgery.
Infection – Infection is a possibility but is rare (1%). You will be given antibiotics as a precaution.
Nerve injury – This is possible but rare.
Malunion: Sometimes the bone may heal in an abnormal position. In some instances the shoulder may continue to function well despite a malunion but if function is affected then further surgery may be considered.
Nonunion: Occasionally the fracture may fail to heal. This may require further surgery.
Stiffness: This is uncommon following injury and surgery. In most instances it will resolve as you start moving the arm with the aid of physiotherapy.
Implant related symptoms: These are uncommon. Further surgery to remove the device is rarely necessary.
Aftercare
Following the procedure the surgical wound is covered with a shower-proof dressing. The dressing should be left undisturbed as far as possible for 14 days. If the dressing is removed for any reason they should be replaced with similar dressing or waterproof plaster. Prior to discharge from hospital a physiotherapist will provide instructions about looking after the shoulder. You will be advised to protect the shoulder by wearing a sling for 4 weeks and intermittently performing movements of the shoulder within certain limits. After 4 weeks you may stop wearing the sling and will be allowed to move the shoulder actively through a greater range. You may resume driving at 2 weeks. Strengthening exercises are started after 8 weeks. Vigorous use of the arm or lifting heavy objects should be avoided for at least 3 months. Outpatient physiotherapy will be arranged and may need to be continued for 3-6 months.
Follow-up
An appointment will be arranged for you to be seen at 2 -4 weeks after the procedure. Follow-up is required for at least 12 months after surgery or until a satisfactory recovery is achieved. X-rays will be performed at intervals to monitor fracture healing.