Alternatives
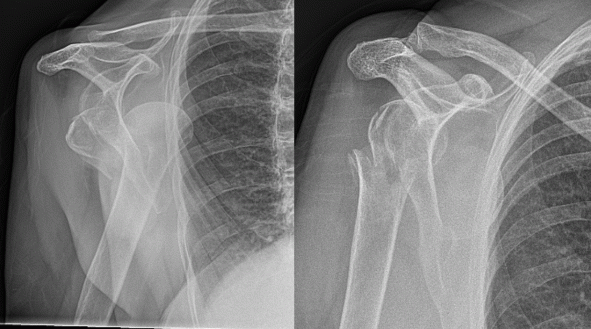
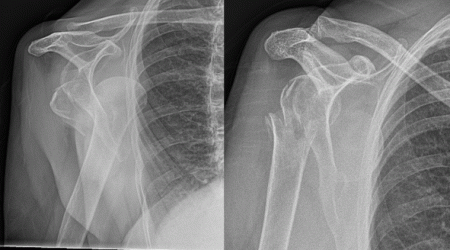
The alternatives for treating a proximal humerus fracture are
a) Allow nature to take its course and have physiotherapy as pain eases
b) operative fixation of the fracture, which may be suitable if the fragments of bone can be realigned and fixed with a plate and screws or an intramedullary nail
c) a partial shoulder replacement (or Hemiarthroplasty), which may be appropriate if the tuberosity fragments are large and can be reconstructed
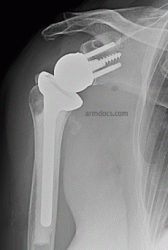
d) a Reverse shoulder replacement, which is appropriate in older individuals in whom it is not possible to accurately reconstruct the fracture.
How is the procedure performed?
A Reverse shoulder replacement is performed under a combination of general and regional anaesthesia. The shoulder is exposed, the humeral head (ball fragment) is removed, a metal hemisphere is fixed on to the socket (glenoid) of the shoulder and a metal prosthesis with a plastic cup insert is implanted in the shaft of the humerus. The tuberosities (bone fragments which carry tendon attachments) are realigned and then fixed to the prosthesis and humeral shaft with sutures or cable. The fixation is supplemented with bone graft using bone from the removed fragment.
Benefits
A Reverse shoulder replacement usually renders the shoulder relatively pain free and allows the use of the arm. It is designed to improve the mechanical efficiency of the deltoid muscle and provide a fulcrum for the joint.
Risks
Medical complications
Chest infection, Deep vein thrombosis, Pulmonary embolism, Myocardial infection are possible after surgery.
Surgical complications
Infection: The risk of infection is 1-3%. Several measures are employed to minimize the risk of infection including administration of antibiotics prior to the operation, an aseptic technique and the use of a clean air theatre.
Nerve injury: This is possible but rare.
Bleeding : Bleeding may occur during or after surgery. A blood transfusion is rarely required. In very rare instances a blood vessel may be damaged as a consequence of injury or surgery.
Tuberosity failure: If the bone is weak due to osteoporosis, the fixation of the tuberosities may fail leading to tuberosity migration. This will inevitably compromise the function of the shoulder. In some instances the bone of the tuberosities may disappear over time.
Stiffness: This is not uncommon following injury and surgery. In most instances it will resolve as you start moving the arm with the aid of physiotherapy.
Instability: The shoulder may dislocate after surgery but this is rare.
Periprosthetic fracture: The shaft of the humerus may fracture during the course of the operation or if there is a further injury after the operation.
Regional pain syndrome: This can occur after fractures or surgery.
Scapular notching: This complication is specific to reverse shoulder replacement and occurs when the humeral component abuts against the scapula (shoulder blade). Progressive notching may sometimes lead to wear of the plastic insert in the joint.
Implant failure: The glenoid component may loosen over time. This may require further surgery.
Revision: If the artificial joint fails then further surgery may be necessary to exchange the joint.
Aftercare
Following the procedure the surgical wound is covered with a shower-proof dressing. The dressing should be left undisturbed as far as possible for 14 days. If the dressing is removed for any reason they should be replaced with similar dressing or waterproof plaster. Prior to discharge from hospital a physiotherapist will provide instructions about looking after the shoulder. You will be advised to protect the shoulder by wearing a sling for 4 weeks and intermittently performing movements of the shoulder within certain limits. After 4 weeks you may stop wearing the sling and will be allowed to move the shoulder actively through a greater range. You may resume driving at 8-12 weeks. Strengthening exercises are started after 12 weeks. Vigorous use of the arm or lifting heavy objects should be avoided for at least 3 months. Outpatient physiotherapy will be arranged and may need to be continued for 6-12 months.
For detailed instructions on rehabilitation after a Reverse shoulder replacement click here.
Follow-up
An appointment will be arranged for you to be seen between 2-6 weeks after the procedure. Follow-up is required for at least 6-12 months after surgery or until a satisfactory recovery is achieved. X-rays will be performed at intervals to monitor tuberosity healing.