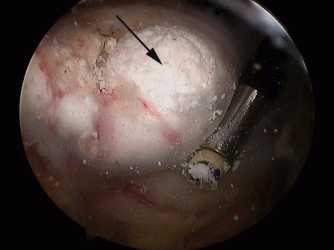
How is the procedure performed?
The procedure is performed under a combination of general and regional anaesthesia. An arthroscope is inserted into the joint and the inside of the joint and subacromial bursa are examined. The calcium deposit is usually identified on the upper surface of the tendon and its location is confirmed by inserting a needle. The tendon overlying the calcium is incised and the calcium is squeezed out and removed. Where a large deposit is removed the defect in the tendon may be repaired with sutures. Other procedures such as subacromial decompression or in some instances a capsular release may be performed, if indicated, at the same time.
Benefits
The main benefit of the procedure is to relieve pain and improve the function of the joint and ability to use the arm. Surgery generally leads to a quicker and earlier resolution of the condition compared with nonsurgical treatment. More than 85% of patients achieve benefit from surgery.
Risks
The overall risk of complications is approximately 15%. The development of a complication may occasionally require further surgery.
Pain - The shoulder may be painful for some weeks after surgery.
Swelling – The shoulder may remain swollen for a day or two after surgery.
Bleeding – A small amount of bleeding from the arthroscopy portal sites is not unusual.
Stiffness – This occurs in approximately 10-15% of patients. Prevention is the key and it is essential to follow the instructions provided, perform daily stretching to maintain the range of movements. If stiffness persists over a number of months, then occasionally further treatment may be necessary.
Recurrence – Once treated, recurrence of calcific tendonitis in the same shoulder is rare.
Infection – Infection is a possibility but is rare after arthroscopic surgery.
Nerve injury, Complex regional pain syndrome, Venous thromboembolism – These are possible but rare.
Aftercare
Following the procedure the arthroscopy portal sites (skin incisions) will be closed with sutures and tape and covered with shower-proof dressings, which should be left undisturbed for 5-7 days. If the dressings are removed for any reason they should be replaced with similar dressings or waterproof plasters. Prior to discharge from hospital a physiotherapist will provide instructions about looking after the shoulder. You will be advised to protect the shoulder by wearing a sling and intermittently performing limited passive/ assisted movements of the shoulder only for 4 -6 weeks. After 6 weeks you will be allowed to move the shoulder actively. Strengthening exercises are started after 12 weeks. Outpatient physiotherapy will be arranged and may need to be continued for 6-9 months.
Resuming activities
You may resume driving at approximately 6 weeks after surgery or when you have regained sufficient movements and control of the arm. Return to work will depend on your occupation. Manual activities should be avoided for at least 4 months. Non-contact sports may be resumed at 4 months.
Follow-up
An appointment will be arranged for you at 2-4 weeks after the procedure. Follow-up is required for at least 6-12 months after surgery or until a satisfactory recovery is achieved.